What is a food allergy? Symptoms, causes and treatment
Last Updated : 28 May 2025Key takeaways:
- Food allergies involve an immune system response to proteins in foods, leading to symptoms such as itchy eyes, shortness of breath, dry mouth, skin redness and hives, abdominal pain, nausea, vomiting, diarrhoea, and in severe cases swelling of the airways and a drop in blood pressure (anaphylaxis).
- Food allergies are most common in children and prevalence decreases with age. Some allergies, such as those to peanuts or tree nuts, are more likely to persist into adulthood.
- There is currently no cure for food allergies. To manage a food allergy, people who are allergic must completely avoid the allergen to avoid adverse reactions.
- Precautionary allergen labels (e.g., ‘may contain’) help consumers identify possible allergens in foods; however, such labelling is currently voluntary in the EU, leading to inconsistencies in how allergen risks are communicated. As a result, ‘may contain’ warnings are used so frequently – and often without clear explanation – that they can be confusing and unhelpful for consumers trying to assess actual risk.
- Efforts are being made to establish threshold levels for allergens, helping to create more consistent and scientifically backed labelling practices, reducing unnecessary warnings and expanding safe food choices.
Food allergies are more common than you might think, and they can range from mild to serious, life-threatening reactions. But what exactly is a food allergy, and how is it different from an intolerance? If you’ve ever wondered why some people have to be so careful about what they eat – or if you suspect you might have a food allergy yourself – this article breaks it all down. From symptoms and triggers to testing and treatment, we’ll cover everything you need to know to stay safe and informed.
What’s the difference between food allergy and intolerance?
A food allergy occurs when an allergen (a protein in a food, which in the majority of people will not produce an adverse reaction) sets off a chain of reactions involving the immune system.1
Food intolerances don’t involve the immune system and are generally less serious than most allergic reactions. They can be due to (i) an enzyme deficiency, e.g. lactase (the enzyme required to digest the milk sugar lactose) which may be produced in low quantities or none at all by people who are lactose intolerant; (ii) pharmacological (e.g. due to amines such as histamine or other compounds such as caffeine), where the body may struggle to metabolize specific compounds in foods that contain high quantities of them or (iii) in some cases the mechanism may be undefined.2
What is an allergic reaction?
An allergic reaction is the response of the body's immune system to normally harmless substances (known as allergens), such as pollens, foods, and house dust mites. When the immune system encounters these substances for the first time, it produces large numbers of antibodies, called IgE antibodies, which bind to the surface of mast cells – a type of immune cell found in tissues throughout the body, especially in the skin, lungs, and digestive tract. This is known as sensitisation. The next time the body encounters that particular allergen, the IgE antibodies on the surface of the mast cells are activated, causing the release of chemicals such as histamine, which cause the allergic symptoms.1
What are the symptoms?
Allergic symptoms can range from mild (causing discomfort), to life threatening. Common symptoms affect the face, skin, respiratory system and the gut. Symptoms affecting the face or skin include a runny or itchy nose, dry mouth, itchy eyes, sneezing, or a rash (itchy red skin or hives). In the windpipe and lungs, allergies can cause wheezing and shortage of breath, and in the gut, symptoms such as abdominal discomfort, nausea, vomiting and diarrhoea may occur.1
A severe allergic reaction is known as anaphylaxis and can be life-threatening. Anaphylaxis causes closing of the throat and difficulty breathing. It may also result in a drop in blood pressure, abdominal pain and vomiting and unconsciousness. People experiencing anaphylaxis should be treated immediately.3
How common are food allergies?
The prevalence of food allergies varies between different ages. In children, 9.3% of the population have a food allergy, which decreases to around 5.0% during adulthood.4 This decline occurs because some children outgrow their allergies, particularly to milk, egg, wheat, and soy, as their immune system develops. However, allergies to peanuts, tree nuts, fish, and shellfish are more likely to persist into adulthood.5
It’s also worth noting that the percentage of people who think they’re allergic (i.e., self-diagnosis) is higher than the percentage of people who are actually diagnosed by health professionals. This discrepancy highlights the need for accurate diagnosis to avoid that people restrict their diets unnecessarily and ensure reliable prevalence data.
Which are the most common allergy-causing foods?
Although many foods or groups of foods can trigger an allergic reaction, 14 of them have been identified as the most common or serious causes of food allergies in the EU. These 14 most common allergens are:6
- Celery
- Gluten
- Crustaceans
- Egg
- Fish
- Lupin
- Milk
- Molluscs
- Mustard
- Peanut
- Sesame seed
- Soybean
- Sulphur dioxide/sulphites
- Tree nuts
Is it possible to develop or lose an allergy during your lifetime?
Most allergies begin in childhood, or as a teenager, but it’s possible to develop an allergy at any point in your life. Childhood allergies can be outgrown later in life, but that isn’t common for late-onset allergies. Mild allergic reactions may become more serious over time, so it’s important to see a doctor even for mild reactions.6
Does an allergic person always experience the same symptoms?
An allergic person will not always experience the same symptoms on different occasions. There are a range of factors (affecting the food or person) which might have an effect on the severity of the reaction on any given day. They include:1
- How the food has been processed (fried, baked, boiled etc.)
- The variability of the food (ripeness, season etc.)
- Sleep
- Menstrual cycle stage
- Psychological factors
- Physical activity
- Cumulative allergen exposure
- Stress
- Infection
- Alcohol usage
- Medication
- Climate
These factors may affect the amount of allergen required to cause a reaction in an individual on different occasions. For example, someone experiencing high levels of stress or drinking alcohol might notice aggravated symptoms following exposure to an allergen compared to a period of calm and sobriety.
How can I find out if I’ve got an allergy?
Doctors use three main testing methods for diagnosing allergies: blood tests, food challenges or elimination tests.7
- Blood tests are often in the form of skin prick tests, where the skin is pricked with a drop of the allergen on it, to see if IgE antibodies are produced (indicating an allergic reaction). Other blood tests measure levels of specific IgE antibodies to suspected or known allergens. The likelihood of a clinical reaction increases with higher IgE levels.
- Food challenge tests involve the patient eating suspected allergenic foods in gradually increasing amounts to see if allergic symptoms occur. These are always conducted under controlled conditions. Sometimes these tests take the form of double-blind placebo-controlled food challenge tests (DBPCFC). This is where neither the subject nor the investigator knows whether the food contains the allergen under investigation.
- In an elimination test, the suspected foods are removed from the diet. If allergic symptoms disappear, suspected foods are gradually reintroduced into the diet in very small quantities while the person is closely monitored for any symptoms. Once all the suspected foods have been checked out, foods causing problems can be avoided.
Is there a cure for a food allergy?
There is currently no cure for food allergies. The condition must be managed by the susceptible individual’s careful avoidance of the allergen-containing food. However, research is being undertaken to try and prevent the initial sensitisation stage in an allergic reaction.
For example, to minimise peanut allergy risk, guidelines recommend introducing peanuts early on when introducing solid foods during complementary feeding.9,10 If your infant has severe eczema, egg allergy, or both (conditions that increase the risk of peanut allergy), introduce peanuts as early as 4 to 6 months of age. If your infant has mild to moderate eczema, it’s recommended to introduce peanuts around 6 months of age. Give peanuts crushed, ground, or try a smooth nut butter to reduce the risk of choking. The amount of peanut protein to be eaten per week should be approximately 6 to 7 grams over 3 or more feedings. One feeding (2 g of peanut protein) looks like, for example, 9-10 g or 2 teaspoons of peanut butter or 8 g or 10 whole peanuts (2 ½ teaspoons of grounded peanuts).10
Guidelines also recommend introducing well-cooked, but not raw egg or uncooked pasteurised, egg during complementary feeding to minimise allergy risk.9 Introduce around 2 g egg protein (approximately 1/3 of an egg) per week to your infants’ diet, starting from 4 to 6 months of life. It’s always best to consult your GP or allergy specialist before introducing peanuts or egg to infant’s diets.
How are food allergies treated?
Food allergies are managed primarily by avoiding the allergenic food which requires careful reading of ingredient labels. If you accidentally ate a food with an allergen, mild reactions may be treated with antihistamines, while severe reactions, such as anaphylaxis, require an epinephrine injection and emergency medical care. Epinephrine is a hormone that acts on the body in several ways. It relaxes the muscles in the lungs which makes it easier to breathe, it constricts blood vessels to counteract the dangerous drop in blood pressure, and it decreases inflammation, preventing the throat from closing. The injection is usually given in the thigh muscle, and its effects start within minutes. After using epinephrine, emergency medical care is still needed.8
Some newer treatments, like immunotherapy, aim to gradually desensitise allergic people by exposing them to small, controlled amounts of the allergen. However, these treatments should be only done under medical supervision.1
If you have a food allergy:8
- Read ingredient labels carefully, even for familiar products, as formulations may change. For foods that are not pre-packaged or foods prepared on-site (e.g., a café or restaurant), staff is required by law to provide information on the ingredients and possible allergens.
- Be cautious when eating out by asking restaurant staff about potential allergens in meals and risk of cross-contamination in the kitchen.
- Avoid cross-contamination by using separate utensils and cookware for allergen-free foods.
- Educate family, friends, and caregivers about specific allergies and emergency response procedures.
- Carry emergency medication (such as an epinephrine auto-injector) if prescribed by a doctor.
- Plan ahead when travelling or attending events, for example by taking safe snacks or meals yourself or by researching restaurants or food options beforehand to find allergy-friendly choices.
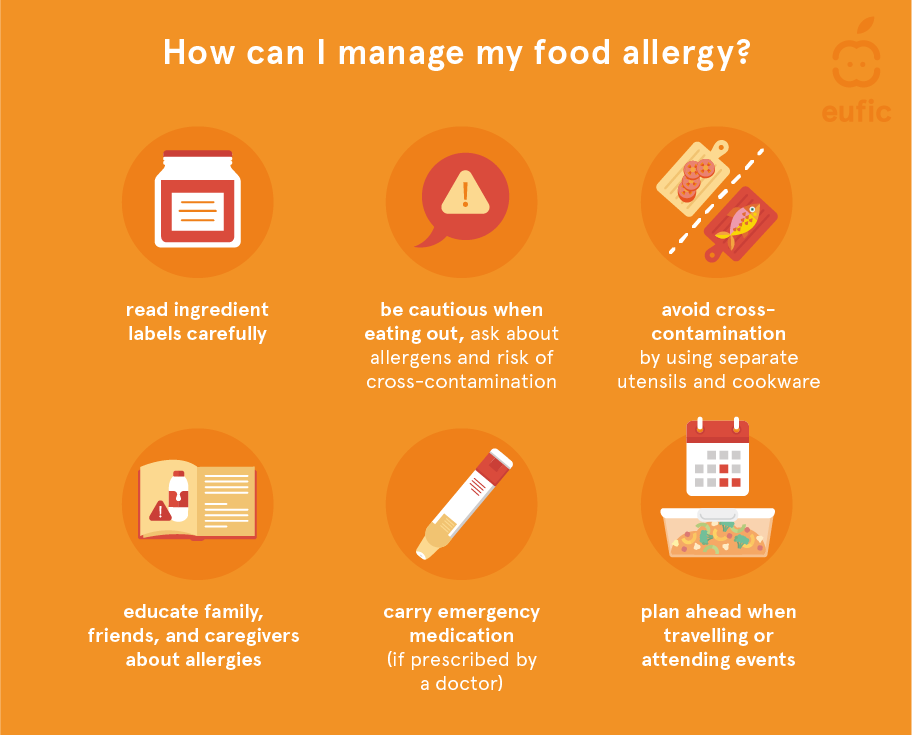
Fig. 1 – How can I manage my food allergy?
How do we know if a food contains an allergen?
To alert consumers to the presence of allergens in food products, food companies use allergen labels. There are two types of allergen labels: mandatory and precautionary.11
Mandatory labels: A compulsory label to alert consumers to the presence of allergenic ingredients. Under EU law, the fourteen allergens listed above must be declared on the label of the foodstuff if they are used as an ingredient (including those carried over in processing aids, additives and solvents).
Precautionary labels: If a priority allergen is not used as an ingredient, but there is a chance that the allergen may be present (through cross contamination), food companies often choose to use a voluntary precautionary label, for example ‘may contain X’, or ‘created in a factory that handles X’.
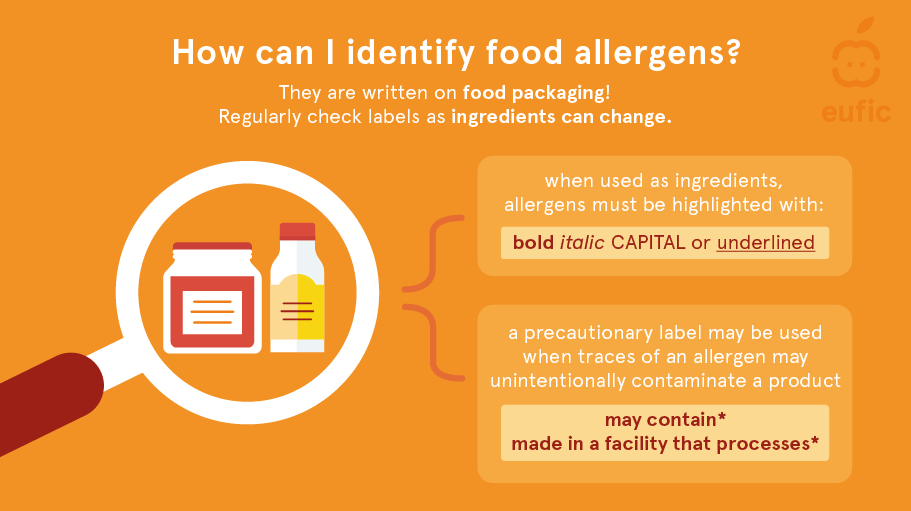
Fig. 2 – How can I identify food allergens?
What are the problems with the current labelling system?
Precautionary allergen labelling (PAL) is not legally regulated in the EU, meaning its use is entirely voluntary and varies between manufacturers. This can make it difficult for allergic consumers to assess how much risk a product actually poses.12
As testing methods have improved, food manufacturers can now detect allergens in increasingly trace amounts. To avoid liability, many companies apply PAL broadly, even when the actual risk of cross-contamination is minimal. This had led to overuse of precautionary warnings, significantly limiting food choices for allergic consumers. While some allergic individuals can tolerate trace amounts of allergens in foods, in others such amounts may still cause an (severe) allergic reaction.
Another ongoing challenge is the lack of clear allergen thresholds – the minimum amount of an allergen that could trigger a reaction in sensitive individuals. Currently, there is no standard across the EU for when a PAL statement should be used. To address this, experts are working on establishing threshold doses based on scientific data. There are also discussions within the EU about harmonising PAL rules to ensure that allergen warning provide clear, evidence-based risk communication, rather than just blanket precaution.
What work is on-going in Europe relating to precautionary labelling?
Efforts are underway in Europe to establish a ‘threshold level’ for different allergens. A threshold level refers to the smallest amount of an allergen that is unlikely to trigger a reaction in most allergic individuals. These scientifically determined, risk-based limits could help create a more consistent approach to precautionary allergen labelling (PAL). Under this system, PAL statements would only be required on foods that may contain allergens at or above the threshold level, while products with contamination level below this threshold would be exempt from such warnings.13
This approach would benefit both food manufacturers and people with food allergies. For manufacturers, it would provide clear guidance on when a PAL statement is necessary, reducing unnecessary precautionary warnings. For consumers, it would mean fewer overly cautious labels, making it easier to identify foods that are truly risky and expanding safe food choices. Ultimately, the goal is to ensure that PAL is based on scientific risk assessment rather than broad precaution, improving both safety and clarity in allergen labelling across Europe.
Conclusion
Living with a food allergy can be challenging, but with the right knowledge and precautions, it’s totally manageable. While there’s no cure yet, science is making strides in allergy research, and clearer food labelling legislation – both in retail and the hospitality sector – is helping people make safer choices. Understanding the difference between food allergies and intolerances, recognising symptoms, and following appropriate precautions are essential steps in managing the condition effectively.
Learn more about the most common food allergens and foods that contain them.
References
- Allergy UK. (2025). What is an allergy? Access 26 March 2025.
- Allergy UK. (2025). Food intolerance. Accessed 26 March 2025.
- Allergy UK. (2025). Anaphylaxis and severe allergic reactions. Accessed 26 March 2025.
- Spolidoro G, et al., (2023). Frequency of food allergy in Europe: an updated systematic review and meta‐analysis. Allergy, 78(2), 351-368.
- Allergy UK. (2025). Top 14 food allergens. Accessed 26 March 2025.
- EFSA NDA Panel (EFSA Panel on Dietetic Products, Nutrition and Allergies), 2014. Scientific Opinion on the evaluation of allergenic foods and food ingredients for labelling purposes. EFSA Journal 2014; 12(11):3894, 286 pp.
- Allergy UK. (2025). Food allergy testing and diagnosing. Accessed 26 March 2025.
- Allergy UK. (2025). Food allergy. Accessed 26 March 2025.
- Halken S, et al. (2021). EAACI guideline: Preventing the development of food allergy in infants and young children (2020 update). Pediatric Allergy and Immunology, 32(5), 843-858.
- Togias A, et al. (2017). Addendum guidelines for the prevention of peanut allergy in the United States: report of the National Institute of Allergy and Infectious Diseases–sponsored expert panel. World Allergy Organization Journal, 10, 1-18.
- European Parliament and Council. (2011). Regulation (EU) No 1169/2011 of the European Parliament and of the Council of 25 October 2011 on the provision of food information to consumers, amending Regulations (EC) No 1924/2006 and (EC) No 1925/2006 of the
- FAO & WHO. 2023. Risk assessment of food allergens – Part 3: Review and establish precautionary labelling in foods of the priority allergens, Meeting report. Food Safety and Quality Series No. 16. Rome.
- ILSI Europe. (2025). Food allergy. Accessed 26 March 2025.


